

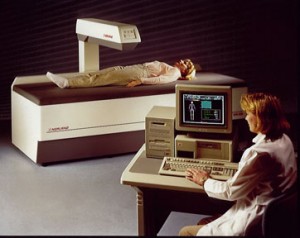
This is in contrast to typical DXA exams in the general population where patients are able to mount the table unassisted, using a stool if needed, with the presence of only 1 staff member. First, to overcome the physical barrier of the tabletop height, we had to have 3 staff members present to assist with lifting subjects from the wheelchair to the scanner table. We identified several logistical barriers to routine BMD assessment in the SCI population. Rooms of this minimum dimension limit entry and maneuverability of stretchers, wheelchairs, and hoyer lifts. All 3 manufacturers suggest a smaller minimum room dimension of 244-320 centimeters by 244-335 centimeters. For both DXA scanners at our facility, the room size measured 375 centimeters by 360 centimeters with a door width of 87 centimeters. Also, the room size again limited maneuverability of this device. But, the design of the DXA scanner prevents placement of the lift close enough to the table for safe transfers because there is no space under the table to position the base and legs of the lift. We also attempted to use a hoyer lift for transfers. However, the room where the DXA scanning was performed was too small for easy entry and maneuvering with a stretcher. To address the difficulties of transferring from wheelchair to the DXA scanner tabletop, we attempted to have subjects transfer from a stretcher to the table. Tabletop heights ranged from 66 centimeters to 76 centimeters from the floor (see table 1), and none was capable of lowering to below 66 centimeters. We then surveyed the table height of several other commonly used DXA scanners and found this to be a universal issue. This height differential is too great for standard sliding board transfers from a wheelchair (see figure 1). First, the height of the DXA scan table used in this study is fixed at 67.5 centimeters, with a differential between a typical wheelchair seat and the table of 15 centimeters. We identified several physical barriers to routine BMD assessment in the SCI population.

Hologic machine specifications were obtained in a similar fashion, with documentation provided by local service representatives.
NORLAND XR 46 SERVICE MANUAL SERIES
General Electric Lunar Prodigy™ and DPX™ series dimensions were obtained from the GE Healthcare internet website, and those for the iDXA™ series through the local sales representative. Cooper Surgical service representatives were contacted for Norland DXA machine documents, which included the footprint specifications and operator's guide. Food and Drug Administration (FDA) and manufactured by General Electric Healthcare (Waukesha, WI), Hologic (Bedford, MA), and Norland (Norland Cooper Surgical Co., Trumbull, CT). These measurements were compared with all models currently approved for use by the U.S. Room dimensions, including door width, were also measured. Measurements of scanning machine dimensions (table height, width, and length) were taken manually with a tape measure for the GE Lunar Prodigy DXA densitometer, and the Hologic QDR system used routinely for clinical (Hologic) and research (GE Lunar) purposes at our facility. Survey of Dimensions of all DXA Machines Approved for Clinical Use
11 Given the lack of SCI patient-specific DXA protocols, in the current study we sought to define barriers to routine bone mineral density (BMD) assessment for individuals with SCI. We have been assessing the health of individuals with spinal cord injury since 1994 as part of an epidemiological study assessing chronic health outcomes in chronic SCI. 4 - 10 Currently, these sites are not included in standardized dual energy x-ray absorptiometry (DXA) protocols designed for osteoporosis screening. In contrast, SCI-associated bone loss and fracture risk are greatest at the metaphyses of the distal femur and proximal tibia. 2, 3 In post menopausal and senile osteoporosis, most clinically relevant fractures occur at the hip, distal radius, and lumbar spine. 1 As many as 70% of individuals with SCI will sustain a long bone fracture at some point following their injury with the mean time to first fracture at 9 years post-injury. Spinal cord injury (SCI) is associated with severe osteoporosis that increases the risk of low-impact fractures (i.e., those that occur in the absence of trauma).
